Behavioral Treatments for Gastrointestinal Disorders
Presented by Laurie Keefer, PhD
Presentation Overview:
Why do we use behavioral therapies in the management of GI conditions?
There are two primary reasons why behavioral therapies are often used in GI conditions. First, GI disorders do not happen in a vacuum- they can affect our entire life, not just our GI tract. Common concerns of GI patients include pain, shame, stigma, sadness, loneliness, fatigue, worry, fear of symptoms or the future and even medical trauma. We also know that the unpredictability of GI symptoms can often make it difficult for patients to make plans or maintain a social network. A behavior therapist might be able to provide extra support around your diagnosis and symptoms and help you manage the intense feelings that come along with it. Further, stress management techniques can help patients who feel their symptoms are made worse by stress.
Brain-gut psychotherapies are also offered by mental health professionals and focus on working with the faulty signaling that develops between the gut and the brain and can amplify symptoms. These therapies are based in similar psychological principles as those that treat depression and anxiety but have been specifically adapted by GI psychologists to improve how the brain is interpreting sensations arising from the gut. These therapies are typically offered by specially trained GI Psychology professionals.
What are some of the brain-gut psychotherapies that may help me?
Basically, any intervention that directly focuses on the way the brain and the gut communicate can be helpful. The most tested brain-gut psychotherapies, meaning they have been shown to improve GI symptoms and quality of life in randomized clinical trials, are Cognitive Behavior Therapy and Gut-Directed Hypnotherapy.
GI- Cognitive behavior therapy (GI-CBT) is a collaborative, brief therapy that connects how you think, feel, and behave in the context of your GI condition. For example, many people find themselves anticipating negative events such as not being able to find a bathroom when needed or may find themselves feeling helpless when abdominal pain comes on. GI-CBT can teach skills that can improve upon these unhelpful beliefs and attitudes and help you focus on what is important to you, helping you re-engage with your life despite your GI symptoms. This type of therapy is often offered over 6-12 sessions over 3-4 months with home practice exercises commonly assigned between visits.
Gut-directed hypnotherapy (GDH) is a relaxation and imagery-based intervention that relies on the subconscious communication between the brain and gut. Once patients are placed in a voluntary hypnotic state, the trained therapist offers symptom-specific, brain-gut related “suggestions” that bypass all of the thoughts and feelings we may have about our condition and helps the brain-gut re-regulate. It is often offered over 7-12 sessions over 3-4 months and usually incorporates home practice between sessions.
How do I find someone in my community?
It can be very difficult to find a mental health professional who understands the brain-gut connection and your GI diagnosis. There are some workarounds.
Once you have chosen a website, you can apply filters that help you narrow in on a therapist who reports they have interest/experience in chronic illness or chronic pain, has had specific training in behavioral medicine, health psychology or medical social work, who describes themselves as CBT oriented or has trained in hypnotherapy. Do not be afraid to call the therapist and ask them about their experience- many will even offer a free 15-minute consultation to see if you are a good fit. You can also encourage your gastroenterologist to reach out to the therapist and explain your condition if you feel comfortable.
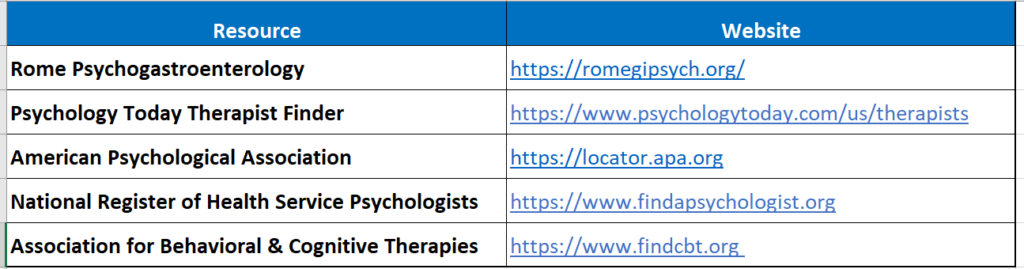
Table 1. Therapist searching websites
About Dr. Keefer:
Laurie Keefer, PhD is a Gastroenterology (GI) Health Psychologist and Professor of Medicine and Psychiatry at the Icahn School of Medicine at Mount Sinai in New York City. She has a more than 20 years of experience in the development and implementation of behavioral therapies for chronic digestive disorders, including IBS, esophageal disorders and Inflammatory Bowel Disease (IBD). She currently directs the GRITT Program, an integrated care model for Crohn’s and ulcerative colitis patients within the IBD Center at Mount Sinai Hospital. She maintains a small clinical practice focused on medically complex IBD.
Her research focuses on the application of positive psychology principles, particularly resilience and acceptance to the management of chronic digestive conditions. She has sustained NIH funding since 2008, including holding the first ever T32 Training grant for young investigators at the intersection of physiology and psychology. She continues to focus on the development of precision-based, scalable GI self-management interventions and recently co-founded Trellus Health, Inc, a digital care solution for the chronic conditions based on her GRITT Methodology.
Dr. Keefer is Founder and Chair of the Rome Foundation’s GastroPsych group and serves on the Board of Directors of the Rome Foundation. She is on the advisory board for the ANMS Research Institute. She has more than 200 peer-reviewed publications and recently co-edited the Handbook of Psychogastroenterology for Mental Health Professionals. Dr. Keefer is a sought-after speaker, mentor and collaborator.
Dr. Keefer received her PhD in clinical psychology from the University of Albany in New York and completed a residency and fellowship in health psychology at Rush University Medical Center in Chicago. She has been a champion for integrated behavioral care in gastroenterology and has trained many in this model around the world. She lives in Northern NJ with her husband, two teens and dog.

