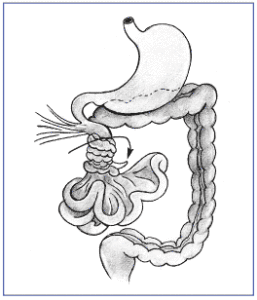
Volvulus is a condition in which the bowel twists on itself, causing obstruction to the flow of material through the bowel. It can also lead to obstruction of the blood supply to the intestine itself, which can result in tissue death within the bowel.[1]
It is most commonly due to a birth defect called malrotation, which is when the bowel becomes misaligned during fetal development. The bowels do not have a normal attachment to the abdominal wall, which makes it possible for the bowels to shift out of their normal position or rotate. It can also occur in the absence of underlying malrotation. If it is associated with malrotation, it often occurs early in life, frequently in the first year.
Symptoms of Volvulus
Infants suffering from this condition experience a sudden onset of symptoms identical to those of bowel obstruction. Symptoms are generally dramatic enough that infants are quickly taken to the emergency room, which can be critical for survival.
Some children with may also experience recurring episodes of vomiting with abdominal pain, which resolve without treatment. This may be due to a condition known as ‘intermittent volvulus,’ which occurs when the bowel just happens to twist, then untwist on its own. [2]
Symptoms that may indicate bowel obstruction due to volvulus include:
- Abdominal tenderness
- Nausea or vomiting
- Vomiting green bile-looking material
- Bloody or dark red stool
- Constipation or difficulty expelling stools
- Distended abdomen
- Shock
Testing
In testing for volvulus, the following tests may be performed:
- A stool sample test finds blood in the stool.
- An upper GI X-ray with small bowel follow-through shows a malrotated bowel or midgut volvulus.
- A CT scan may show evidence of intestinal obstruction.
- A barium enema often shows an abnormal position of the bowel, suggesting malrotation.
- Blood tests to check the electrolytes may show abnormalities.
If the volvulus is intermittent, a clinician may suspect its presence just from a history of repeated, occasional, self-resolving symptoms. Even if it is not present during testing, an upper GI series may show that the junction of the duodenum and jejunum are misplaced, or a barium enema may identify that the cecum is not in the right lower quadrant where it should be. Both of these findings are indicative of malrotation, which may indicate intermittent volvulus.[2]
Treatment
Emergency surgery is necessary to repair a volvulus. An incision is made in the abdominal wall, and the bowels are untwisted and the blood supply restored. If a small segment of bowel is necrotic (dead from lack of blood flow), it is removed and the ends of the healthy bowel are sewn back together, or used to form a colostomy or ileostomy (a tube to the outside through which bowel contents can be removed — the term depends on where the tube is placed). If the entire bowel is necrotic, the outlook is poor and life-threatening.
Early recognition of the volvulus and prompt treatment generally results in a good outcome. If necrosis of the bowel occurs the prognosis is often poor, depending on how much of the bowel is necrotic.
Possible complications include:
- Secondary peritonitis (infection of the abdomen) may occur if the volvulus and subsequent obstruction causes a bowel perforation.
- Short bowel syndrome may occur if a large part of the small bowel has to be removed due to tissue death.
Learn more about Disorders of the Colon and Rectum
References
[1] All material adapted from Medline Plus: Volvulus – childhood, except as otherwise noted.
[2] Yamamoto, LG. Malrotation and Volvulus. Chapter X.5, Case Based Pediatrics For Medical Students and Residents. Department of Pediatrics, University of Hawaii, John A. Burns School of Medicine (2003).
