
This page includes news on developments in drug treatments for chronic gastrointestinal illnesses. No endorsement is intended or implied.
To find clinical trials and other research studies currently recruiting participants, click here
Treatment News
Developments in drug treatments for functional GI and motility disorders.
2026
January 2026 — Sebela Pharmaceuticals® Announces Submission of New Drug Application to FDA for Tegoprazan for the Treatment of Gastroesophageal Reflux Disease: BRAINTREE, Mass., Jan. 12, 2026 /PRNewswire/ — Braintree Laboratories, Inc. a part of Sebela Pharmaceuticals® and a leading manufacturer of gastroenterology pharmaceutical products, announced that it submitted a New Drug Application (NDA) on January 9, 2026 to the U.S. Food and Drug Administration (FDA) for tegoprazan, a novel potassium-competitive acid blocker (P-CAB), for the treatment of adults with gastroesophageal reflux disease (GERD). The NDA seeks simultaneous approval for three indications: treatment of heartburn associated with non-erosive reflux disease (NERD), healing of erosive esophagitis (EE), and maintenance of EE healing.
The NDA submission is supported by robust data from the pivotal Phase 3 TRIUMpH clinical program, which enrolled over 2,000 US patients and demonstrated tegoprazan’s clinical superiority over a PPI across multiple endpoints. Read full press release here
January 2026 —Vanda Pharmaceuticals Announces FDA Approval of NEREUS™ (tradipitant) for the Prevention of Vomiting Induced by Motion: A Historic Scientific Milestone in the Prevention of Motion Sicknes WASHINGTON, Dec. 30, 2025 /PRNewswire/ — Vanda Pharmaceuticals Inc. (Vanda) (Nasdaq: VNDA) today announced that the U.S. Food and Drug Administration (FDA) has approved NEREUS™ (tradipitant), an oral neurokinin-1 (NK-1) receptor antagonist, for the prevention of vomiting induced by motion. This approval marks the first new pharmacologic treatment in motion sickness in over four decades, representing a significant advancement in the understanding and management of this debilitating physiologic response that affects a substantial portion of the population and has long been recognized as a factor affecting military operational readiness. Read full press release here
2025
November 2025 — Vanda Pharmaceuticals Reports Positive Results for Tradipitant in Preventing GLP-1 Induced Nausea and Vomiting: WASHINGTON, Nov. 17, 2025 /PRNewswire/ — Vanda Pharmaceuticals Inc. (Vanda) (Nasdaq: VNDA), a leading biopharmaceutical company focused on the development and commercialization of innovative therapies, today announced positive topline results from its randomized controlled clinical study (VP-VLY-686-2601) evaluating tradipitant, an oral neurokinin-1 (NK-1) receptor antagonist, for the prevention of nausea and vomiting induced by GLP-1 receptor agonist Wegovy® in overweight and obese adults.
This study, which pre-treated patients with either tradipitant or placebo before administering a 1 mg injection of Wegovy®, a dose that normally takes 9 weeks of titration to reach, succeeded and met its primary endpoint, with only 29.3% of tradipitant-treated participants (17/58) experiencing vomiting compared to 58.6% on placebo (34/58) (p=0.0016), representing a 50% relative reduction. The study also met the key secondary endpoint of the proportion of participants with vomiting and significant nausea at 22.4% in the tradipitant group (13/58) versus 48.3% on placebo (28/58) (p=0.0039).
Tradipitant demonstrated a favorable safety profile consistent with previous studies with no new safety signals observed. Read full press release here

October 2025 — mBIOTA Elemental Diet Named to TIME 2025 Best Inventions List Santa Monica, October 9, 2025 : mBIOTA Labs, a medical food company revolutionizing the field of therapeutic nutrition, today announced that its flagship product, mBIOTA Elemental™ Diet, was named to the TIME 2025 Best Inventions List for its novel solution for chronic GI disorders. mBIOTA Elemental™ Diet is the first clinically proven and highly palatable medical food designed for the nutritional management of gastrointestinal (GI) dysfunction, including small intestinal bacterial overgrowth (SIBO), intestinal methanogen overgrowth
(IMO), irritable bowel syndrome (IBS), inflammatory bowel diseases (IBD), and eosinophilic esophagitis (EoE). The science-backed formula, developed in partnership with leading gastroenterologist researchers and food scientists, delivers complete nutrition while providing relief and remission for patients suffering through painful GI disorders.
“mBIOTA Labs is beyond thrilled that our first product is included in TIME’s list of Best Inventions and has proven itself as an incredibly impactful medical solution both clinically and in the real world,” said Krystyna Houser, founder of mBIOTA Labs. “This honor is a testament to our rigorous, science-based work and advocacy for a better experience for the millions of individuals who currently struggle with GI symptoms without a truly viable solution. We look forward to continuing this momentum as we grow our clinical vision and footprint across new use cases for palatable elemental diets.” Read Full Press Release Here
August 2025 — BRAINTREE, Mass., Aug. 7, 2025 /PRNewswire/ — Braintree Laboratories, a part of Sebela Pharmaceuticals® and a leading manufacturer of gastroenterology pharmaceutical products, today announced positive topline results from the 24-week maintenance phase of the pivotal Phase 3 TRIUMpH clinical program evaluating tegoprazan, a novel potassium-competitive acid blocker (P-CAB), in gastroesophageal reflux disease (GERD). See Full Press Release Here
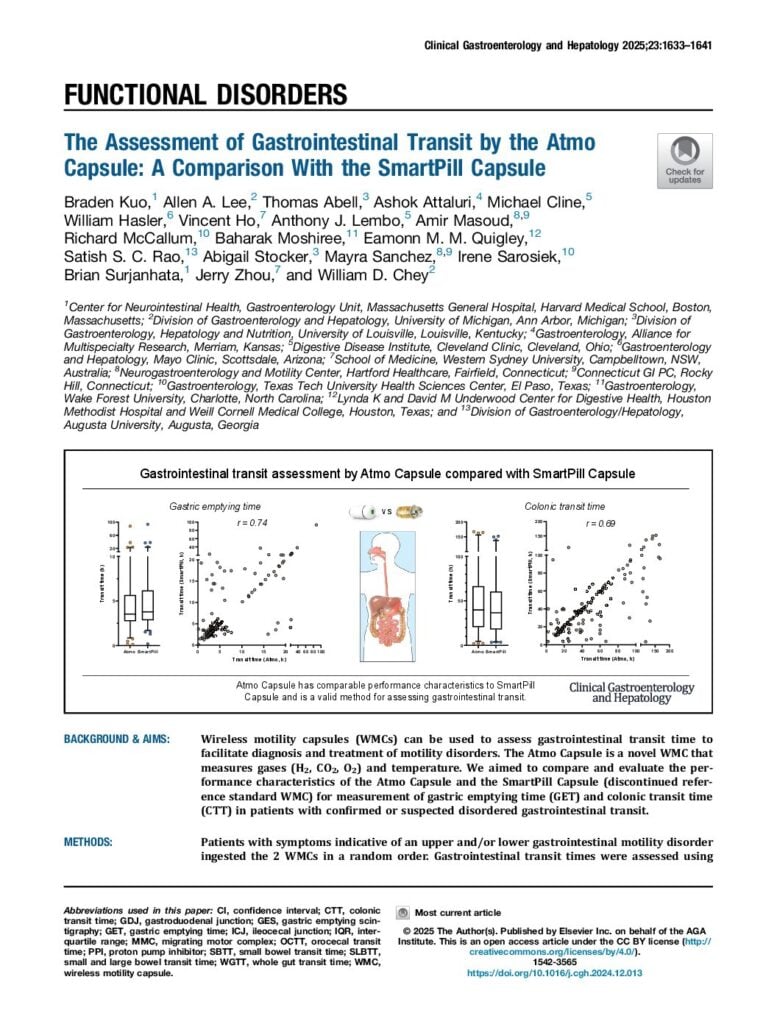
July 2025 — Atmo Biosciences receives US FDA clearance for ingestible gas-sensing capsule
MELBOURNE, AUSTRALIA & SAN DIEGO, USA, 27 June 2025: Atmo Biosciences, a leader in ingestible capsule technology, is delighted to announce that it has received US Food and Drug Administration (FDA) 510(k) clearance for the Atmo Gas Capsule System, paving the way for its first product to be marketed and sold in the USA. This breakthrough milestone is another significant step in Atmo’s commercial execution plan to bring the product to a wider audience of healthcare providers and patients globally.
July 2025 — SUFFERN, N.Y., July 24, 2025 (Newswire.com) – CDx Diagnostics announced today that the U.S. Food and Drug Administration (FDA) granted Breakthrough Device Designation for its proprietary WATS3D diagnostic system, a ‘first-of-a-kind’ AI-powered digital pathology system using wide area transepithelial sampling for the diagnosis of Barrett’s esophagus and early neoplastic alterations in patients at risk for disease progression.
“The Breakthrough Device Designation recognizes what the volume of clinical data has shown: the WATS3D Test improves the ability to detect dysplasia in Barrett’s esophagus, offering patients and physicians an improved method of detection of patients at risk of development of esophageal cancer,” said Robert Odze, MD, a leading gastrointestinal pathologist.
May 2025 — BOSTON–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), a biotechnology company developing and commercializing life-changing therapies for people living with gastrointestinal (GI) and rare diseases, today announced that, based on a recent discussion with the U.S. Food and Drug Administration (FDA), a confirmatory Phase 3 trial is needed to seek approval of apraglutide for patients with short bowel syndrome (SBS) with intestinal failure (IF) who are dependent on parenteral support. While continuing to advance apraglutide, Ironwood has engaged Goldman Sachs & Co. LLC to explore strategic alternatives for the company to maximize value for stockholders.
In preparation for the new drug application (NDA) submission, pharmacokinetic analysis indicated that the exposure and dose delivered in the STARS Phase 3 trial were lower than planned due to dose preparation and administration. Based on the strength of the STARS Phase 3 results, Ironwood believed that there was a regulatory path forward. However, following recent dialogue with the FDA it became clear that a confirmatory Phase 3 trial is needed to seek approval. Ironwood plans to work with the FDA on the design of a confirmatory Phase 3 trial and the regulatory path forward.
Apraglutide generated strong safety and efficacy data in the STARS Phase 3 trial, the largest SBS-IF trial to date, and, following an analysis of long-term extension trial data, 27 apraglutide-dosed patients dependent on parenteral support achieved enteral autonomy, which is the ultimate goal for these patients. Consistent with FDA discussions, Ironwood plans to continue the long-term extension trial and believes the data from the STARS trial will continue to be an integral part of an NDA submission package.
April 2025 — BRAINTREE, Mass., April 23, 2025 /PRNewswire/ — Braintree Laboratories, a part of Sebela Pharmaceuticals® and a leading manufacturer of gastroenterology pharmaceutical products, today announced positive topline results from two pivotal US Phase 3 clinical trials evaluating tegoprazan, a novel potassium-competitive acid blocker (P-CAB), in patients with gastroesophageal reflux disease (GERD).
Across both the EE and NERD pivotal studies known as TRIUMpH, tegoprazan achieved significance in all primary and secondary endpoints tested. This included statistical superiority over a PPI (lansoprazole) in achieving complete esophageal healing at weeks 2 and 8 across all grades of EE, including the significant cohort of patients with severe disease (LA Grades C & D). In the NERD trial, tegoprazan demonstrated complete symptom relief for both heartburn (overnight and heartburn free days) and regurgitation.
The maintenance phase of the EE study will complete in Q3 2025 with a New Drug Application inclusive of both the EE and NERD indications planned for filing with FDA in Q4 2025. Braintree® intends to submit results from the TRIUMpH Phase 3 studies to a high impact, peer reviewed journal along with presentation of this data at a leading gastroenterology conference in the future.
April 2025 — Santa Monica, CA – April 9, 2025 – mBIOTA Labs, an emerging medical food company revolutionizing medical nutrition for the management of gastrointestinal (GI) conditions, is quickly earning industry attention from healthcare professionals and patients alike for their proprietary palatable elemental diet, mBIOTA Elemental™. This clinically-proven and effective solution for patients with small intestinal bacterial overgrowth (SIBO), intestinal methanogen overgrowth (IMO), and similar GI dysfunctions completed a clinical trial at Cedar Sinai Los Angeles in late 2023 and is now available directly to consumers.
mBIOTA Labs completed their first prospective clinical trial assessing both the efficacy and palatability of the mBIOTA Elemental™ diet in patients with SIBO, IMO, or a combination of the two. Patients exclusively consumed mBIOTA Elemental™ diet for two weeks and multiple endpoints were examined before, during and after. Not only did 100% prefer the taste of mBIOTA Elemental™ diet over the current market leader, but eradication rates were higher than expected, significantly outperforming traditional treatments. Full trial results were published in the peer reviewed AGA journal Clinical Gastroenterology & Hepatology.
Archived Industry Treatment News
2024
September 2024 — The U.S. Food and Drug Administration (FDA) approved a label update for GATTEX® (teduglutide) for Injection. GATTEX is a glucagon-like peptide-2 (GLP-2) analog indicated for the treatment of adults and pediatric patients 1 year of age and older with short bowel syndrome (SBS) who are dependent on parenteral support.
The updated U.S. Prescribing Information (USPI) includes new information about the evaluation and testing prior to starting GATTEX treatment and additional monitoring during GATTEX treatment. The changes focus on evaluating and monitoring adult and pediatric patients for small bowel neoplasia using upper gastrointestinal (GI) endoscopy (or alternate imaging).
Healthcare providers who prescribe GATTEX are being informed about the label update. Patients should reach out to their healthcare providers with any questions they have about their treatment.
August 2024 — SOLANA BEACH, Calif., Aug. 08, 2024 (GLOBE NEWSWIRE) — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused primarily on treatments for gastrointestinal (GI) diseases with an emphasis on GIMOTI® (metoclopramide) nasal spray, together with EVERSANA™, a leading provider of global commercial services to the life science industry, joins the gastroparesis community in recognizing Gastroparesis Awareness Month throughout August and supporting the millions of people living with gastroparesis or suffering from associated symptoms of the condition. Established by the International Foundation for Gastrointestinal Disorders (IFFGD) and recognized each year in August by IFFGD and other organizations, Gastroparesis Awareness Month is intended to acknowledge the challenges of living with gastroparesis – symptom burdens, identifying right therapeutic options, and lifestyle modifications while helping to educate patients and their loved ones on managing the condition. Read full press release here.
August 2024 — Takeda Pharmaceuticals- OnePath is now called Takeda Patient Support. There is no change to the services patients are currently receiving. Takeda Patient Support specialists are still here to help with access to prescribed Takeda treatment. Learn more here.
June 2024 —FLORHAM PARK, N.J., July 18, 2024 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal (GI) diseases, announced today the U.S. Food and Drug Administration (FDA) has approved VOQUEZNA® (vonoprazan) 10 mg tablets for the relief of heartburn associated with Non-Erosive Gastroesophageal Reflux Disease (Non-Erosive GERD) in adults. Non-Erosive GERD represents a substantial segment of the U.S. GERD population, affecting millions of individuals suffering from frequent heartburn. This is the third FDA approval for VOQUEZNA, which is also approved to treat all severities of Erosive Esophagitis (EE), also referred to as Erosive GERD, and in combination with antibiotics for the eradication of Helicobacter pylori (H. pylori) infection. Read full press release here.
May 2024 — WASHINGTON, May 15, 2024 /PRNewswire/ — Vanda Pharmaceuticals Inc. (Vanda) (Nasdaq: VNDA) today announced the results from its second Phase III study of tradipitant in motion sickness, confirming the previously reported results of two efficacy studies demonstrating that tradipitant is effective in the prevention of vomiting associated with motion sickness. This Phase III study was conducted in real-world conditions on boats in the coastal waters of the United States (U.S.). View full press release here
February 2024 — BOSTON–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), a GI-focused healthcare company, today announced positive topline results from its pivotal Phase III STARS trial, which evaluated the efficacy and safety of once-weekly subcutaneous apraglutide in reducing parenteral support (PS) dependency in adult patients with short bowel syndrome with intestinal failure (SBS-IF). SBS-IF, a rare and severe organ failure condition in which patients are dependent on PS, affects an estimated 18,000 adult patients in the U.S., Europe, and Japan. Based on these results, Ironwood plans to submit a new drug application (NDA) and other regulatory filings for apraglutide for use in adult patients with SBS who are dependent on PS. View full press release here
February 2024 — Phathom Pharmaceuticals Announces VOQUEZNA® (vonoprazan) Tablets for Erosive GERD and Associated Heartburn Added to Express Scripts National Formularies for Commercial Patients. Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases, today announced the placement of VOQUEZNA® (vonoprazan) tablets for the treatment of adults with Erosive Esophagitis, commonly referred to as Erosive GERD (gastroesophageal reflux disease), and relief of heartburn associated with Erosive Esophagitis on the Express Scripts national formularies, effective immediately. VOQUEZNA is the first and only FDA-approved potassium-competitive acid blocker (PCAB) and the first new class of Erosive GERD treatment to become available in the United States in over 30 years. Commercial access for VOQUEZNA tablets is now estimated at 60 million covered lives in the United States. View Full Press Release Here
February 2024 — FDA Approves Takeda’s EOHILIA (budesonide oral suspension), the First and Only Oral Treatment in the U.S. for Eosinophilic Esophagitis (EoE) (TSE:4502/NYSE:TAK) today announced that the U.S. Food and Drug Administration (FDA) has approved EOHILIA (budesonide oral suspension), the first and only FDA-approved oral therapy for people 11 years and older with eosinophilic esophagitis (EoE).1 It will be available in 2 mg/10 mL convenient, single-dose stick packs by the end of February. View Full Press Release Here
January 2024 — AbbVie and Ironwood are excited to announce that data from the Phase III study that evaluated linaclotide in children and adolescents aged 6-17 years with functional constipation has been published in The Lancet Gastroenterology & Hepatology.
The data highlights efficacy endpoints from the company’s pivotal Phase III trial, which formed the basis of the June 2023 U.S. Food and Drug Administration (FDA) approval of linaclotide for the treatment of functional constipation in 6-17 year olds.
This data led to the FDA-approved prescription drug in the U.S. to treat pediatric functional constipation and will provide clinicians with valuable information to make well-informed prescribing decisions for this pediatric population. Read the published manuscript here
2023
November 2023 — FLORHAM PARK, N.J., Nov. 01, 2023 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal (GI) diseases, announced today the U.S. Food and Drug Administration (FDA) has approved VOQUEZNA® (vonoprazan) tablets 10 mg and 20 mg, a novel potassium-competitive acid blocker (PCAB), as a new treatment for adults for the healing of all grades of Erosive Esophagitis, also known as Erosive GERD (gastroesophageal reflux disease), maintenance of healing of all grades of Erosive GERD, and relief of heartburn associated with Erosive GERD. Read full press release here
June 2023 — FLORHAM PARK, N.J., June 12, 2023 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases, today announced that the U.S. Food and Drug Administration (FDA) has acknowledged that its New Drug Application (NDA) resubmission for vonoprazan, a novel first-in-class potassium-competitive acid blocker (PCAB), for the treatment of Erosive GERD (gastroesophageal reflux disease) constitutes a complete response to the February 2023 complete response letter (CRL). The FDA has classified this as a Class 2 resubmission and assigned a Prescription Drug User Fee Act (PDUFA) goal date of November 17, 2023. Read full press release here.
June 2023 — BOSTON–(BUSINESS WIRE)–Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), a GI-focused healthcare company, today announced that the U.S. Food and Drug Administration (FDA) has approved LINZESS® (linaclotide) as a once-daily treatment for pediatric patients ages 6-17 years-old with functional constipation. LINZESS is the first and only FDA-approved prescription therapy for functional constipation in this patient population. Earlier this year, the FDA granted a 6-month priority review to our supplemental New Drug Application (sNDA), 4 months earlier than the standard review timeline. LINZESS is developed and marketed by AbbVie and Ironwood Pharmaceuticals in the United States. Read full press release here.
June 2023 — CAMBRIDGE, Mass. & HOBOKEN, N.J.–(BUSINESS WIRE)–Jun. 5, 2023– Seres Therapeutics, Inc. (Nasdaq: MCRB) and Nestlé Health Science today announced that VOWST™ (fecal microbiota spores, live-brpk) is now commercially available for patients. VOWST, formerly called SER-109, is the first and only U.S. Food and Drug Administration (FDA)-approved orally administered microbiota-based therapeutic to prevent recurrence of C. difficile infection (CDI) in adults following antibacterial treatment for recurrent CDI (rCDI). VOWST is not indicated for the treatment of CDI. Read full press release here
June 2023 — Effective June 1, 2023, Mahana IBS is transitioning our dispensing pharmacy from Blink HealthⓇ to a new Mahana pharmacy experience supported by CaryRxⓇ. This change will greatly enhance your patient’s checkout experience by reducing the time, effort and steps required to purchase their Mahana IBS prescription. A few notable advantages include:
- Elimination of the need to create a pharmacy customer account
- Streamlined checkout experience
- Reduced time to receive prescription unlock
May 2023 — NORTH CHICAGO, Ill., May 25, 2023 /PRNewswire/ — AbbVie (NYSE: ABBV) today announced the New England Journal of Medicine (NEJM) published results from the pivotal Phase 3 clinical trials – U-EXCEL, U-EXCEED and U-ENDURE – evaluating upadacitinib (RINVOQ®) in adult patients with moderately to severely active Crohn’s disease who have had an inadequate response, lost response or were intolerant to conventional therapy or a biologic agent. Read full press release here
May 2023 — FLORHAM PARK, N.J., May 23, 2023 (GLOBE NEWSWIRE) Phathom Pharmaceuticals Resubmits Erosive GERD New Drug Application to FDA: Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases, today announced that it has resubmitted its New Drug Application (NDA) for vonoprazan, a novel first-in-class potassium-competitive acid blocker (PCAB), for the treatment of Erosive GERD (gastroesophageal reflux disease), also referred to as erosive esophagitis, to the U.S. Food and Drug Administration (FDA). Read full press release
May 2023 — BOSTON and BASEL, Switzerland – May 22, 2023 – Ironwood Pharmaceuticals, Inc. (“Ironwood”) (Nasdaq: IRWD), a GI-focused healthcare company, and VectivBio Holding AG (“VectivBio”) (Nasdaq: VECT), a clinical-stage biopharmaceutical company pioneering novel, transformational treatments for severe rare gastrointestinal conditions, today announced that they have entered into a definitive agreement for Ironwood to acquire VectivBio for $17.00 per share in an all-cash transaction with an estimated aggregate consideration of approximately $1 billion, net of VectivBio cash and debt (the “Transaction”). The acquisition price represents a premium of 80% relative to the volume-weighted average share price over the previous 90 trading days. The Transaction was approved by both the Ironwood and VectivBio Boards of Directors and the Transaction Agreement was entered into on May 21, 2023. The Transaction is conditioned upon, among other things, the tender of shares representing more than 80% of VectivBio’s issued and outstanding shares and other customary conditions. Orbimed, Forbion and Versant Ventures, and VectivBio’s directors and officers, jointly representing 28.6% of VectivBio’s shareholdings, entered into tender and support agreements pursuant to which such supporting shareholders agreed, among other things, to tender their shares in the tender offer. Read the full press release here.
May 2023 — NORTH CHICAGO, Ill., May 18, 2023 /PRNewswire/ — AbbVie (NYSE: ABBV) today announced that the U.S. Food and Drug Administration (FDA) has approved RINVOQ® (upadacitinib) for the treatment of adults with moderately to severely active Crohn’s disease who have had an inadequate response or intolerance to one or more TNF blockers.1 This is the seventh FDA approval for RINVOQ across rheumatology, dermatology, and gastroenterology, where it is now indicated in both ulcerative colitis and Crohn’s disease. Read full press release here
May 2023 — WALTHAM, Mass., May 17, 2023 (GLOBE NEWSWIRE) — Ardelyx, Inc. (Nasdaq: ARDX), a biopharmaceutical company founded with a mission to discover, develop and commercialize innovative, first-in-class medicines that meet significant unmet medical needs, today announced that the U.S. Food and Drug Administration (FDA) has accepted its resubmission of a New Drug Application (NDA) for XPHOZAH® (tenapanor) for the control of serum phosphate in adult patients with chronic kidney disease on dialysis who have had an inadequate response or intolerance to a phosphate binder therapy. The FDA has determined that the NDA is a class 2 review, which results in a six-month review period from the date of resubmission. The FDA has set a user fee goal date of October 17, 2023. The company expects XPHOZAH to be commercially available in the fourth quarter of 2023, as soon as possible following an approval from the FDA. Read full press release here
May 2023 — CAMBRIDGE, Mass.–(BUSINESS WIRE)–May 9, 2023– Seres Therapeutics, Inc. (Nasdaq: MCRB), a leading microbiome therapeutics company, today reported initial clinical data about SER-155. SER-155 is an oral, cultivated bacterial consortia investigational therapeutic designed to prevent enteric-derived infections and resulting blood stream infections, as well as induce immune tolerance responses to reduce the incidence of graft-versus-host disease (GvHD) in patients undergoing allogeneic hematopoietic stem cell transplantation (allo-HSCT). Gastrointestinal (GI) microbiome data from the first 100 days post HSCT in Cohort 1 of the SER-155 Phase 1b open-label study showed the successful engraftment of SER-155 bacterial strains and a substantial reduction in the cumulative incidence of pathogen domination, a biomarker associated with the risk of serious enteric infections and bloodstream infections, as well as GvHD. The tolerability profile observed was favorable, with no serious adverse events attributed to SER-155 administration. Enrollment in the placebo-controlled Cohort 2 portion of the study is ongoing and topline results are anticipated in mid-2024. Read full press release here
May 2023 — BOSTON–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), a GI-focused healthcare company, presented findings during the 2023 Digestive Disease Week® (DDW) meeting from a Phase III clinical trial on the potential of linaclotide for children and adolescents ages 6-17 years-old with functional constipation. Ironwood had previously announced topline data from this study in September 2022. Read full press release here
April 2023 — CAMBRIDGE, Mass. & HOBOKEN, N.J.–(BUSINESS WIRE)–Apr. 26, 2023– Seres Therapeutics, Inc. (Nasdaq: MCRB) and Nestlé Health Science today announced the U.S. Food and Drug Administration (FDA) approval of VOWSTTM (fecal microbiota spores, live-brpk), formerly called SER-109, an orally administered microbiota-based therapeutic to prevent recurrence of C. difficile Infection (CDI) in adults following antibacterial treatment for recurrent CDI (rCDI). VOWST is not indicated for the treatment of CDI. Read full press release here
April 2023 — WALTHAM, Mass., April 18, 2023 (GLOBE NEWSWIRE) — Ardelyx, Inc. (Nasdaq: ARDX), a biopharmaceutical company founded with a mission to discover, develop and commercialize innovative, first-in-class medicines that meet significant unmet medical needs, today announced the resubmission of a New Drug Application (NDA) to the U.S. Food and Drug Administration (FDA) for the approval of XPHOZAH (tenapanor) for the control of serum phosphate in adult patients with chronic kidney disease on dialysis who have had an inadequate response or intolerance to a phosphate binder therapy. An Acknowledgement of Receipt letter from the FDA, confirming the resubmission is complete, is expected in mid-May. We expect that the letter will include the classification of the resubmission and the review goal date. Read full press release here
April 2023 — LAVAL, QC / ACCESSWIRE / April 4, 2023 / Bausch Health Companies Inc. (NYSE:BHC)(TSX:BHC) and its gastroenterology (GI) business, Salix Pharmaceuticals, today announced the results from the third edition of its patient perspectives survey, an annual survey of U.S. adults living with irritable bowel syndrome (IBS) or chronic idiopathic constipation (CIC). The report, Patient Perspectives: Impacts of Living with IBS, offers a current understanding of the behaviors and experiences of the IBS and CIC patient population, including insights on diagnosis, barriers to provider discussions, and symptom management. Learn more
March 2023 — BASEL, Switzerland, March 13, 2023 (GLOBE NEWSWIRE) — VectivBio Holding AG (“VectivBio”) (Nasdaq: VECT), a clinical-stage biopharmaceutical company pioneering novel transformational treatments for severe rare conditions, and Asahi Kasei Pharma Corporation (“Asahi Kasei Pharma”) today announced the start of a Phase 1 study investigating the pharmacokinetics, pharmacological action, safety, and tolerability of apraglutide when a single subcutaneous dose is given to healthy Japanese adult men and women. Pharmacological actions and safety will be investigated by comparison with a placebo control. Read full press release here
February 2023 — CAMBRIDGE, Mass.–(BUSINESS WIRE)–Feb. 14, 2023– Seres Therapeutics, Inc. (Nasdaq: MCRB), a leading microbiome therapeutics company, today announced the publication of data from its Phase 3 ECOSPOR IV trial (ClinicalTrials.gov Identifier: NCT03183128) in JAMA Network Open that reinforce previously published results from the Phase 3 ECOSPOR III study on the investigational microbiome therapeutic SER-109 for the prevention of recurrent C. difficile infection (rCDI). With nearly 156,000 cases in the U.S., rCDI is a leading cause of hospital-acquired infection and places a significant burden on the healthcare system. See full press release here
February 2023 — LAVAL, QC / ACCESSWIRE / February 13, 2023 /Bausch Health Companies Inc. (NYSE/TSX:BHC) today announced the opening of the 2023 Salix Gastrointestinal Health Scholars Program application period. The program will award 10 exceptional students living with GI disease a scholarship of up to $10,000 as they work to pursue their higher education goals. See full press release here
February 2023 — CAMBRIDGE, Mass.–(BUSINESS WIRE)–Feb. 8, 2023– Seres Therapeutics, Inc. (Nasdaq: MCRB), a leading microbiome therapeutics company, today announced that enrollment in Cohort 2 in its SER-155 Phase 1b study is underway. SER-155, an investigational oral microbiome therapeutic, is designed to reduce the incidence of gastrointestinal (GI) infections, bloodstream infections, and graft versus host disease (GvHD) in individuals undergoing allogeneic hematopoietic stem cell transplantation (allo-HSCT). See full press release
February 2023 — BOSTON–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), a GI-focused healthcare company, today announced that the U.S. Food and Drug Administration (FDA) has granted Priority Review to the supplemental New Drug Application (sNDA) for LINZESS® (linaclotide) for the treatment of children and adolescents ages 6-17 years-old with functional constipation (FC). The FDA has assigned the application a Prescription Drug User Fee Act (PDUFA) date of June 14th, 2023, four months earlier than the standard review cycle. See full press release here
January 2023 — FLORHAM PARK, N.J., Jan. 08, 2023 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases and disorders, announced today positive topline results from PHALCON-NERD-301, a Phase 3 study evaluating the efficacy and safety of vonoprazan for the daily treatment of adults in symptomatic non-erosive gastroesophageal reflux disease (sGERD or NERD). Vonoprazan is an investigational first-in-class potassium-competitive acid blocker (PCAB) from a novel class of medicines that block acid secretion in the stomach. Full results from the study are expected later this year. See full press release here
January 2023 — OSAKA, Japan, CAMBRIDGE, Massachusetts, and Pasadena, CALIF., Jan. 9, 2023 – Takeda (TSE:4502/NYSE:TAK) and Arrowhead Pharmaceuticals Inc. (NASDAQ: ARWR) today announced topline results from the Phase 2 SEQUOIA clinical study of investigational fazirsiran (TAK-999/ARO-AAT) for the treatment of liver disease associated with alpha-1 antitrypsin deficiency (AATD-LD). The companies also provided an outline of a Phase 3 study that was co-developed by Takeda and Arrowhead and will be conducted by Takeda. Additional SEQUOIA study results are planned to be presented at a future medical meeting and submitted for publication. Arrowhead will host a webcast call for investors today, January 9, 2023, at 8:30 a.m. ET to review the Phase 2 data. Read full press release here
January 2023 — FLORHAM PARK, N.J., Jan. 03, 2023 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases and disorders, today announced that the U.S. Food and Drug Administration (FDA) has notified the Company that no action will be taken on the Company’s new drug application (NDA) for vonoprazan, a novel potassium-competitive acid blocker (PCAB), under review as a treatment for erosive esophagitis, on or prior to the current Prescription Drug User Fee Act (PDUFA) target action date of January 11, 2023. See full press release here
2022
December 2022 — NORTH CHICAGO, Ill., Dec. 16, 2022 /PRNewswire/ — AbbVie (NYSE: ABBV) today announced that it has submitted a supplemental New Drug Application (sNDA) for linaclotide (LINZESS®) to the U.S. Food and Drug Administration (FDA) for the treatment of children and adolescents 6 to 17 years of age with functional constipation (FC). The sNDA submission is based on results from a Phase 3 clinical trial, which met the primary and secondary endpoints, evaluating linaclotide (72 mcg) for increased frequency of spontaneous bowel movements (SBM) and improvement in stool consistency in patients aged 6 to17 years. LINZESS is developed and marketed by AbbVie and Ironwood Pharmaceuticals in the United States and is currently indicated for the treatment of adults with chronic idiopathic constipation (CIC) or irritable bowel syndrome with constipation (IBS-C). Learn more
December 2022 — SOLANA BEACH, Calif., Dec. 07, 2022 (GLOBE NEWSWIRE) — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused primarily on treatments for gastrointestinal (GI) diseases with an emphasis on GIMOTI® (metoclopramide) nasal spray, today announced that the United States Patent and Trademark Office (USPTO) issued US patent No. 11,517,545 under the title “Treatment of Moderate and Severe Gastroparesis.” Read full press release here
October 2022 — FLORHAM PARK, N.J., Oct. 24, 2022 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases and disorders, today announced it has completed enrollment in its PHALCON-NERD Daily Dosing Phase 3 trial of vonoprazan in non-erosive gastroesophageal reflux disease (NERD). Vonoprazan is an investigational first-in-class potassium-competitive acid blocker (PCAB) from a novel class of medicines that block acid secretion in the stomach. The Company expects to share topline data from the primary endpoint in the first quarter of 2023 and full results from the study in late 2023.
If successful, Phathom believes that the trial will form the basis of a supplemental New Drug Application (sNDA) for vonoprazan as once daily therapy for the treatment of symptomatic NERD in adults in 2023.
October 2022 — FLORHAM PARK, N.J., Oct. 23, 2022 (GLOBE NEWSWIRE) — Phathom Pharmaceuticals, Inc. (Nasdaq: PHAT), a biopharmaceutical company focused on developing and commercializing novel treatments for gastrointestinal diseases and disorders, announced today that detailed results from an investigational Phase 2 study evaluating the efficacy of vonoprazan in non-erosive gastroesophageal reflux disease (NERD) and other data will be presented at the American College of Gastroenterology (ACG) 2022 Annual Scientific Meeting, being held October 21-26 in Charlotte, NC. Read full press release here.
September 2022 — BOSTON, Mass.–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (Nasdaq: IRWD), today announced positive topline data from a Phase III clinical trial evaluating LINZESS (linaclotide) 72 mcg in pediatric patients aged 6-17 with functional constipation (FC). The trial met its primary and secondary endpoints, demonstrating that linaclotide (72 mcg) improved frequency of spontaneous bowl movements (SBM) and stool consistency. Linaclotide was generally well-tolerated, and the safety profile is consistent with previously reported studies with linaclotide in FC and irritable bowel syndrome (IBS) in pediatric patients. See full press release here
September 2022 — CAMBRIDGE, Massachusetts, September 14, 2022 Takeda (TSE:4502/NYSE:TAK) today announced the national launch of the CDPATHTM program, which includes an innovative, validated personalized prognostic tool that uses blood tests† to help predict the potential risk of developing serious Crohn’s disease-related complications within three years.1,2 CDPATH is available for use by US-based physicians and offered at no cost to eligible patients††, providing an opportunity for patients to partner with their physicians to map out a personalized disease management plan.
CDPATH is for adult patients (≥18 years old) diagnosed with Crohn’s disease (CD) within the past 10 years who have yet to experience serious complications defined as bowel strictures, internal penetrating disease, or non-perianal surgery (bowel resection or stricturoplasty).1,2 Patients can have blood drawn for the CDPATH test at one of more than 2,500 participating locations nationwide. Read the full press release here
August 2022 — SOLANA BEACH, Calif., Aug. 01, 2022 (GLOBE NEWSWIRE) — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused on treatments for gastrointestinal (GI) diseases, today announced their ongoing collaboration with the International Foundation for Gastrointestinal Disorders (IFFGD) for Gastroparesis Awareness Month celebrated in August each year. Alongside the IFFGD, Evoke and EVERSANA’s goal for the month is to help improve general understanding and awareness of gastroparesis to help patients and families manage the condition. See full press release here
August 2022 — CAMBRIDGE, Mass., Aug. 31, 2022 /PRNewswire/ — Kiwi Biosciences, the Y Combinator-funded biotech startup making food painless, launches the next generation FODZYME®, a novel patent-pending enzyme supplement helping people enjoy their favorite foods, wherever they are. Low-FODMAP certified by Monash University, FODZYME breaks down common gut symptom triggers found in garlic, onion, wheat and other popular foods. These compounds, called FODMAPs, are particularly problematic for people with Irritable Bowel Syndrome (IBS), which affects 15% of the global population. See full press release here.
June 2022 — Auckland, New Zealand, Wednesday 15 June, 2022. Alimetry, a medical device and digital healthcare company, today announced it has received US Food and Drug Administration (FDA) clearance for Gastric Alimetry, a pioneering non-invasive medical device for aiding the diagnosis gastric disorders. Alimetry also announced today the launch of Alimetry Inc., a subsidiary based in Minneapolis, MN, that will market and distribute Gastric Alimetry in the United States.
June 2022 — CAMBRIDGE, Mass.–(BUSINESS WIRE)–Jun. 13, 2022– Alnylam Pharmaceuticals, Inc. (Nasdaq: ALNY), the leading RNAi therapeutics company, today announced that the U.S. Food and Drug Administration (FDA) approved AMVUTTRA™ (vutrisiran), an RNAi therapeutic administered via subcutaneous injection once every three months (quarterly) for the treatment of the polyneuropathy of hereditary transthyretin-mediated (hATTR) amyloidosis in adults. hATTR amyloidosis is a rare, inherited, rapidly progressive, and fatal disease with debilitating polyneuropathy manifestations, for which there are few treatment options. The FDA approval is based on positive 9-month results from the HELIOS-A Phase 3 study, where AMVUTTRA significantly improved the signs and symptoms of polyneuropathy, with more than 50 percent of patients experiencing halting or reversal of their disease manifestations. View the full release here.
April 2022 — Ardelyx, Inc. (Nasdaq: ARDX), a biopharmaceutical company founded with a mission to discover, develop and commercialize innovative first-in-class medicines that meet significant unmet medical needs, today announced the launch of IBSRELA, the first and only NHE3 inhibitor for the treatment of irritable bowel syndrome with constipation (IBS-C) in adults. IBSRELA is the first FDA-approved product for Ardelyx. View the press release here. You can also view the Full Prescription Information, including the box warning here.
February 2022 — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused primarily on treatments for gastrointestinal (GI) diseases with an emphasis on Gimoti (metoclopramide) nasal spray (GIMOTI), today announced that the results of a retrospective analysis of United States (US) administrative claims data that examined the association between tardive dyskinesia (TD) and potential risk factors will be presented at the annual Digestive Disease Week Meeting in San Diego, CA taking place from May 21-24, 2022.
Selected as a poster of distinction during DDW 2022, the presentation titled: “Revisiting the Risk of Tardive Dyskinesia with Metoclopramide Use: A Real-World Data Driven Epidemiology Study From 2011-2021” will cover the data analytics of an 80 million patient database (Truven Health MarketScan®) used to conduct the most comprehensive analysis to date on the risk of metoclopramide-induced tardive dyskinesia. In the limited literature available, the reported incidence of TD varies widely.
Details of the poster presentation are as follows:
Session Title: Gastroparesis and Small Intestinal Dysmotility
Presentation Title: “Revisiting the Risk of Tardive Dyskinesia with Metoclopramide Use: A Real-World Data Driven Epidemiology Study From 2011-2021”
Date: May 21, 2022
Time: 12:30 p.m. – 1:30 p.m. PDT
Location: San Diego Convention Center
2021
December 2021— BOSTON (December 8, 2021) Next-Generation Cellvizio delivers real-time, in vivo cellular imaging to address growth in life-threatening, high-cost disease states. A timely, accurate diagnosis is the difference between life and death for millions of people who are diagnosed with complex conditions like cancer, respiratory disease, and gastrointestinal disease. As the occurrence of these conditions continues to grow, the ability to quickly and accurately deliver a diagnosis and determine the best course of treatment is more important than ever. Cellvizio® from Mauna Kea Technologies supports this need with the only confocal laser endomicroscopy (CLE) device that allows physicians to see real-time cellular activity virtually anywhere in the human body. Mauna Kea Technologies, which has received 19 U.S. FDA 510(k) clearances for its technology, achieved its most recent FDA clearance for its Next-Generation Cellvizio platform in August 2021. Cellvizio has proven to be effective in diagnosing and informing the treatment of deadly diseases like lung cancer, pancreatic cysts, and esophageal cancer (EAC); as well as functional conditions such as irritable bowel syndrome (IBS), and food intolerance.,, Cellvizio has also been cleared for use in a range of procedures, including gastrointestinal endoscopy, bronchoscopy, surgical and robot-assisted procedures. For more information, visit www.maunakeatech.com.
September 2021 — Azurity Pharmaceuticals is recalling one lot of Firvanq (vancomycin hydrochloride for oral solution), Vancomycin 50 mg/mL Kit because some products in the affected lot have been found to incorrectly contain a First Omeprazole (FIRST-PPI) diluent instead of the Firvanq diluent bottle. Vancomycin may not be completely solubilized in the FIRST-PPI diluent which could lead to doses above or below those recommended in the label. There is reasonable probability that the administration of inappropriate doses of oral vancomycin may lead to persistent diarrhea associated with dehydration and electrolyte abnormalities, recurrence of Clostridium difficile (C. difficile) infection, its progression to severe colitis, colon perforation requiring colectomy, and potentially death. Especially, the elderly and immunocompromised patients are vulnerable to the complications of C. difficile infection. Read recall here.
July 2021 — LeadCare II, LeadCare Plus, and LeadCare Ultra Blood Lead Tests by Magellan Diagnostics: Class I Recall – Due to Risk of Falsely Low Results. Magellan Diagnostics, is recalling its LeadCare II, LeadCare Plus, and LeadCare Ultra Blood Lead Tests due to a significant risk of falsely low results. The FDA has significant concerns that the performance of the test may provide falsely low results and may lead to health risks in special populations such as young children and pregnant individuals. A pregnant or lactating individual’s exposure to lead is concerning because it not only may cause health problems for the parent but can result in lead exposure to the developing baby. Obtaining falsely low results may lead to patient harm including delayed puberty, reduced postnatal growth, decreased IQ, and inattention and behavior problems in children. Read recall here.
June 22, 2021 — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused on treatments for gastrointestinal (GI) diseases, and EVERSANA™, a leading provider of global commercial services to the life science industry and The International Foundation for Gastrointestinal Disorders’ (IFFGD), today announced its membership into IFFGD Industry Council. Evoke will join a likeminded group of organizations and brands focused on bettering patients affected by gastrointestinal disorders. As part of the Industry Council, Evoke will participate in bi-annual council meetings to gain industry insights and provide feedback on future plans for IFFGD.
In addition to the Industry Council, Evoke is excited to sponsor the IFFDG’s upcoming 30th Anniversary Digestive Health Virtual Walk in August during Gastroparesis Awareness Month. This walk is a unique fitness event which will provide participants with an opportunity to engage at their own pace and as their health and schedules permit. To honor the thirty years of the IFFGD’s existence, the overall campaign goal is for all participants to collectively walk 10,950 miles over two weeks. Goals will also go beyond physical fitness by encouraging participants to participate in activities that promote general wellness such as scheduling a doctor’s appointment, trying a new gut friendly recipe or starting a log of their meals and/or symptoms.
June 22, 2021 — Mauna Kea Technologies (Euronext: MKEA) inventor of Cellvizio®, the multidisciplinary probe and needle-based confocal laser endomicroscopy (p/nCLE) platform, today announces a peer-reviewed publication in the journal Nature Scientific Reports entitled “Cross-sectional imaging of intestinal barrier dysfunction by confocal laser endomicroscopy can identify patients with food allergy in vivo with high sensitivity” (2021, https://www.nature.com/articles/s41598-021-92262-4). This paper provides new evidence that Cellvizio®, thanks to its unique capability to perform real-time functional imaging in vivo and at the cellular level, can accurately diagnose patients with food allergies. Learn more.
June 15, 2021 — ATLANTA, June 15, 2021 /PRNewswire/ — ModifyHealth, together with Monash University, Australia, announce a partnership that will seek to raise further awareness in the US of the FODMAP diet protocol and the Monash University FODMAP Diet App, which have helped millions of people manage irritable bowel syndrome (IBS). The partnership will increase engagement with US consumers and healthcare providers, and expand awareness of the latest research and developments of the FODMAP diet protocol. Learn more
June 14, 2021 — Meters Biopharma, Inc. (NASDAQ:NMTR), a clinical-stage biotechnology company focused on rare and unmet needs in gastroenterology, announced today the initiation of its Phase 2 trial of vurolenatide, a proprietary long-acting glucagon-like peptide-1 (GLP-1) agonist in adults with short bowel syndrome (SBS). The Phase 2 trial, known as the VIBRANT (VurolenatIde for short Bowel syndrome Regardless of pArenteral support requiremeNT) study, is a double-blind, multicenter, placebo-controlled parallel group study of the safety, efficacy and tolerability of vurolenatide in adult patients with short bowel syndrome. Read more about this phase 2 study here.
June 2021 —Viona Pharmaceuticals Inc., is voluntarily recalling 2 (two) lots of Metformin Hydrochloride Extended-Release Tablets, USP 750 mg to the retail level. The 2 (two) lots of Metformin Hydrochloride Extended-Release Tablets, USP 750 mg have been found to contain levels of Nitrosodimethylamine (NDMA) impurities above acceptable daily limits. This product was manufactured by Cadila Healthcare Limited, Ahmedabad, India in November 2019, for U.S. distribution by Viona Pharmaceuticals Inc. Read more about this recall here.
May 31, 2021 — BOSTON–(BUSINESS WIRE)– Ironwood Pharmaceuticals, Inc. (NASDAQ: IRWD), a GI-focused healthcare company, presented new findings at the Digestive Disease Week® (DDW) 2021 virtual meeting from a survey highlighting disease burden and care-seeking behavior among adult patients with irritable bowel syndrome with constipation (IBS-C) during the COVID-19 pandemic.
The poster presentation, titled Disease Burden and Care-Seeking Behavior for IBS-C Patients in the United States in the Era of COVID-19(presentation number Fr014), summarized data from a cross-sectional online general health survey of 130 adults with IBS-C conducted from August through October 2020. More than a third of surveyed IBS-C patients indicated their symptoms had worsened during the COVID-19 pandemic. Additionally, nearly a quarter reported cancelling healthcare visits due to COVID-19. Also, nearly half (46%) of surveyed IBS-C patients reported that they did not seek care from a healthcare provider in the past year for their symptoms.
Other key findings from the survey, which was conducted in collaboration with researchers from the Mayo Clinic, the Acumen Health Research Institute and the International Foundation for Functional Gastrointestinal Disorders, include:
- Surveyed IBS-C patients reported a significantly higher proportion of moderate-to-severe anxiety and depression and significantly lower health-related quality of life (HRQoL) than surveyed patients without IBS-C.
- Absenteeism and presenteeism were also significantly higher among surveyed IBS-C patients versus those without IBS-C.
- 25% of surveyed IBS-C patients reported currently taking a prescription medication whereas 68.5% reported currently taking an OTC for their IBS-C symptoms.
- Most common bothersome symptoms in the past seven days included abdominal discomfort, abdominal pain, straining, abdominal bloating and incomplete bowel movements.
May 20, 2021 — During this year’s Digestive Disease Week (DDW) annual meeting, Takeda Pharmaceuticals presented data from several studies of Entyvio® (vedolizumab), including real-world data from the EVOLVE study and GEMINI 2 post-hoc analyses in patients with Crohn’s disease (CD). For more details, please see the two presentations below:
- Real-World Effectiveness of First-Line Biologic Vedolizumab in Crohn’s Disease: Analysis of Higher Treatment Effect Subpopulation from the EVOLVE Study1 – Presentation 22
- The aim of this analysis was to identify a subpopulation of biologic therapy-naïve patients with CD for whom vedolizumab would have a larger treatment effect versus anti-tumor necrosis factor-α (anti-TNFα) therapies for the outcome of clinical remission. Data was analyzed from EVOLVE, a multi-country, retrospective cohort study of patients with inflammatory bowel disease (IBD) who initiated first-line biologic treatment with vedolizumab or anti-TNFα therapy.i
- Results from the EVOLVE study were also recently published in The Journal of Crohn’s and Colitis.
- Symptomatic Improvement with Vedolizumab Therapy for Crohn’s Disease Stratified by Disease Activity and Prior Tumor Necrosis Factor Antagonist Failure: Post Hoc Analyses from the GEMINI 2 Trial2 – Presentation Sa083
The aim of this analysis was to investigate symptomatic improvement, including onset of action, across disease activity and prior anti-TNFα status in patients with CD from the GEMINI 2 phase 3, randomized, placebo-controlled clinical trial of vedolizumab treatment for moderate to severe CD. ii
May 17, 2021 — Ironwood Pharmaceuticals, Inc. (NASDAQ:IRWD), a GI-focused healthcare company, today announced that the company and its collaborators will present seven posters- four of which have been named posters of distinction- during the Digestive Disease Week ® (DDW) 2021 Virtual Meeting. Two posters of distinction will discuss the impact of linaclotide on visceral hypersensitivity, one of the main underlying causes of irritable bowel syndrome with constipation (IBS-C). Other data will discuss disease burden and care-seeking behavior among patients with IBS-C during the COVID-19 pandemic. Additional posters will reveal data from a GI disease survey of nearly 90,000 Americans.
April 12, 2021 — 9 Meters Biopharma, Inc. (NASDAQ:NMTR), a clinical-stage company focused on rare and unmet needs in gastroenterology, announced today that the Company will collaborate with the Celiac Disease Foundation (CDF) to support clinical trial enrollment in 9 Meters’ Phase 3 study, CeDLara, for their drug candidate larazotide in celiac disease. Learn more
February 10, 2021 — Takeda Pharmaceutical Company Limited (TSE:4502/NYSE:TAK) (“Takeda”) today announced that it has submitted an application to the Japanese Ministry of Health, Labour and Welfare to manufacture and market darvadstrocel (development code: Cx601) for the treatment of complex perianal fistulas in adult patients with non-active/mildly active luminal Crohn’s disease (CD).2020
January 31, 2020 — The US Food and Drug Administration (FDA) has approved Dificid (fidaxomicin) tablets and oral suspension for the treatment of pediatric patients with Clostridioides difficile (C. difficile), a bacterium that causes diarrhea and colitis. For more information, please see here.
February 10, 2020 — Palette Life Sciences, Inc., a medical device company dedicated to assisting healthcare professionals (HCPs) to improve patient outcomes in colorectal urologic and oncologic conditions and diseases, today announced the launch of the Solesta® Reimbursement Assistance Program. Solesta is a minimally-invasive, and easily injectable viscous gel made from two polysaccharides, Non-Animal Stabilized Hyaluronic Acid (NASHA®) and Dextranomer (Dx) microspheres.1 Solesta is the only quick, nonsurgical treatment for fecal incontinence, administered in an outpatient setting without the need for anesthesia.2 HCPs can simply follow three steps at MySolesta.com to become trained in Solesta administration and technique. Studies have shown that Solesta can help patients return to a more active lifestyle (socializing, going to work, etc.) and reduces the depression and embarrassment that is often associated with bowel control problems.
February 13, 2020 — The US Food and Drug Administration (FDA) has approved a new treatment for chronic idiopathic constipation (CIC). The approval allows Braintree Laboratories to move forward with lactitol (Pizensy), an osmotic laxative indicated for the treatment of CIC in adults for a recommended dosage of 20 grams orally daily.
February 14, 2020 — Takeda Pharmaceutical Company Limited (TSE:4502/NYSE:TAK) (“Takeda”) today announced results from the phase 3 VISIBLE 2 clinical trial evaluating the efficacy and safety of an investigational subcutaneous (SC) formulation of the gut-selective biologic vedolizumab (Entyvio®) for use during maintenance therapy in adult patients with moderately to severely active Crohn’s disease (CD). The study evaluated patients who achieved clinical response* at week 6 following two doses of open-label vedolizumab intravenous (IV) induction therapy at weeks 0 and 2.[1] The results show that at week 52, significantly more patients on vedolizumab SC compared to placebo were in clinical remission (48.0% [n=132/275] vs. 34.3% [n=46/134] respectively; [p=0.008]),** meeting the study’s primary endpoint.1 These data were announced during an oral presentation at the 15th Congress of the European Crohn’s and Colitis Organisation (ECCO) in Vienna, Austria.February 25, 2020 — WASHINGTON/PRNewswire/ — Vanda Pharmaceuticals Inc. (Vanda) (Nasdaq:VNDA) today announced results from a Phase III clinical trial (EPIONE) of tradipitant for the treatment of pruritus in atopic dermatitis (AD) in adults. The EPIONE study did not meet its primary endpoint in reduction of pruritus across the overall study population. However, the antipruritic effect of tradipitant was robust in the mild AD study population. Mild AD represents over 60% of the total AD population in the U.S.1, 2 The EPIONE study continued to demonstrate that tradipitant is safe and well-tolerated.
March 9th, 2020 — TEL-AVIV, Israel and RALEIGH, N.C., RedHill Biopharma Ltd. (Nasdaq: RDHL) (“RedHill” or the “Company”), a specialty biopharmaceutical company focused on gastrointestinal diseases, today announced the U.S. commercial launch of Talicia® (omeprazole magnesium, amoxicillin and rifabutin)1 delayed-release capsules 10 mg2/250 mg/12.5 mg for the treatment of Helicobacter pylori (H. pylori) infection in adults. RedHill’s expanded U.S. sales force will promote Talicia® nationwide to approximately 25,000 gastroenterologists, primary care physicians and other healthcare providers.
March 24, 2020 — FDA is informing health care providers and patients of the potential risk of transmission of SARS-CoV-2 virus by the use of fecal microbiota for transplantation (FMT) and that FDA has determined that additional safety protections are needed.Several recent studies have documented the presence of SARS-CoV-2 ribonucleic acid (RNA) and/or SARS-CoV-2 virus in stool of infected individuals. This information suggests that SARS-CoV-2 may be transmitted by FMT, although the risk of such transmission is unknown. At this time, testing nasopharyngeal specimens from stool donors for SARS-CoV-2 may not be widely available. Furthermore, there is limited information on the availability and sensitivity of direct testing of stool for SARS-CoV-2.As the scientific community learns more about SARS-CoV-2 and COVID-19, FDA will provide further information as warranted.
April 1, 2020 — The U.S. Food and Drug Administration today announced it is requesting manufacturers to withdraw all prescription and over-the-counter (OTC) ranitidine drugs from the market immediately. This is the latest step in an ongoing investigation of a contaminant known as N-Nitrosodimethylamine (NDMA) in ranitidine medications (commonly known by the brand name Zantac). The agency has determined that the impurity in some ranitidine products increases over time and when stored at higher than room temperatures and may result in consumer exposure to unacceptable levels of this impurity. As a result of this immediate market withdrawal request, ranitidine products will not be available for new or existing prescriptions or OTC use in the U.S.
“The FDA is committed to ensuring that the medicines Americans take are safe and effective. We make every effort to investigate potential health risks and provide our recommendations to the public based on the best available science. We didn’t observe unacceptable levels of NDMA in many of the samples that we tested. However, since we don’t know how or for how long the product might have been stored, we decided that it should not be available to consumers and patients unless its quality can be assured,” said Janet Woodcock, M.D., director of the FDA’s Center for Drug Evaluation and Research. “The FDA will continue our efforts to ensure impurities in other drugs do not exceed acceptable limits so that patients can continue taking medicines without concern.”April 15, 2020— The U.S. Food and Drug Administration has announced that Amneal Pharmaceuticals, LLC, Bridgewater, New Jersey is voluntarily recalling three lots of Nizatidine Oral Solution, 15 mg/mL (75 mg/5mL), packaged in 480 mL bottles to the Consumer Level. This recall is due to potential N-Nitrosodimethylamine (NDMA) amounts exceeding the levels established by the FDA. Read the full announcement here.
April 16, 2020 — The U.S. Food and Drug Administration Center for Drug Evaluation and Research (CDER) announced approval today of Drug Safety-related Labeling Changes for Movantik (NALOXEGOL OXALATE). These changes were made to the Warnings and Precautions, and Adverse Reactions. Read the labeling changes here.
April 28, 2020 — The U.S. Food and Drug Administration has announced that GSK Consumer Healthcare is voluntarily recalling specific lots of Benefiber Healthy Shape Prebiotic Fiber Supplement powder and Benefiber Prebiotic Fiber Supplement powder due to possible plastic contamination from the bottle cap. Read the full announcement, including lot numbers, here.
May 15, 2020 — Today, the U.S. Food and Drug Administration approved Qinlock (ripretinib) tablets as the first new drug specifically approved as a fourth-line treatment for advanced gastrointestinal stromal tumor (GIST), a type of tumor that originates in the gastrointestinal tract. Qinlock is indicated for adult patients who have received prior treatment with three or more kinase inhibitor therapies, including imatinib. Read more here.
June 19, 2020 — SOLANA BEACH, Calif., (GLOBE NEWSWIRE) — Evoke Pharma, Inc. (NASDAQ: EVOK), a specialty pharmaceutical company focused on treatments for gastrointestinal (GI) diseases, today announced that the U.S. Food and Drug Administration (FDA) has approved the New Drug Application (NDA) for GIMOTI™ (metoclopramide) nasal spray, the first and only nasally-administered product indicated for the relief of symptoms in adults with acute and recurrent diabetic gastroparesis. For more information, visit here.
July 13, 2020 —Vanda Pharmaceuticals Inc. (Vanda) (NASDAQ: VNDA) announced today that the U.S. Food and Drug Administration (FDA) has authorized a single patient in an Individual Patient Expanded Access protocol (VP-VLY-686-3303). This patient had previously participated in a randomized study of tradipitant in gastroparesis for 12 weeks. The patient and treating physician requested expanded access to continue treatment beyond 12 weeks, as the treating physician had judged that tradipitant was the only treatment that effectively managed the patient’s gastroparesis symptoms. For more information, visit here.
July 28, 2020 — TEL AVIV, Israel and RALEIGH, NC, RedHill Biopharma Ltd. (Nasdaq: RDHL) (“RedHill” or the “Company”), a specialty biopharmaceutical company, today announced the publication of data from its previously announced Phase 2 study of RHB-102 (Bekinda®)1, a novel, proprietary, once-daily, 12mg bimodal-release ondansetron, in diarrhea-predominant irritable bowel syndrome (IBS-D), in The American Journal of Gastroenterology.
Aug 7, 2020 — Today, the U.S. Food and Drug Administration approved Olinvyk (oliceridine), an opioid agonist for the management of moderate to severe acute pain in adults, where the pain is severe enough to require an intravenous opioid and for whom alternative treatments are inadequate. Olinvyk is indicated for short-term intravenous use in hospitals or other controlled clinical settings, such as during inpatient and outpatient procedures. It is not indicated for at-home use. Here you can read more.September, 2020 — The New Digital Care App to Effectively Manage IBS by Regulating the Gut-Brain Connection- Zemedy is the world’s first evidence-based programme that uses CBT digitally to restore gut-brain connection and help IBS sufferers. A trial V1 of the app was launched in 2019 where it was reported that users experienced a significant reduction in symptoms, some with no flareups at all. Zemedy is from Bold Health, an organisation that creates digital care tools for digestive health. Chronic digestive problems are common and often connected to poor mental wellbeing. Therefore, through its digital applications, Bold Health provides patients with constant access to cognitive behavioural therapy programmes designed for their specific condition.
2019
May 17, 2019 — The US Food and Drug Administration (FDA) has approved an extended indication for the drug teduglutide in pediatric patients one year and older with short bowel syndrome (SBS). Teduglutide was originally approved for use in adults with SBS in 2012.
April 5, 2019 — Following approval by the US Food and Drug Administration (FDA) last year, Takeda Pharmaceuticals has announced that prucalopride (Motegrity), a once-daily, oral treatment for adults with chronic idiopathic constipation (CIC), is now commercially available by prescription in the US.
April 2, 2019 — The US Food and Drug Administration (FDA) has approved the reintroduction of tegaserod (Zelnorm), a twice-daily oral treatment for irritabble bowel syndrome with constipation (IBS-C) in women under 65, following a complete safety review.
February 18, 2019 — A new treatment for fecal incontinence in individuals with spinal cord injury (RDD-0315) was given fast track designation by the US Food and Drug Administration. “Fast track” is a type of designation given by the FDA to expedite the review of investigational therapies which treat a serious or life-threatening condition and fill an unmet medical need.
January 18, 2019 — The National Medical Products Administration (NMPA) has approved linaclotide (Linzess) for the treatment of adults with irritable bowel syndrome with constipation (IBS-C) in China.2018
December 21, 2018 — The US Food and Drug Administration (FDA) has approved an app (InterStim smart programmer) that assists patients using the InterStim system, a therapy providing sacral neuromodulationfor the treatment of overactive bladder or chronic bowel incontinence. The app allows individuals with the InterStim system to manage their treatment at home and gives physicians greater personalization of care.
December 17, 2018 — The US Food and Drug Administration (FDA) has approved prucalopride (Motegrity), a once-daily, oral treatment option for adults with chronic idiopathic constipation (CIC).
December 6, 2018 — Health Canada has approved the antibiotic rifaximin (Zaxine) for the treatment of adults with irritable bowel syndrome with diarrhea (IBS-D) in Canada.
December 6, 2018 — Positive Phase II study results were announced for tradipitant for the treatment of gastroparesis. The drug met the primary endpoint of the study (reduced nausea) and was found to be well tolerated compared with placebo.
December 4, 2018 — The European Commission has granted Orphan Drug Designation to apraglutide for the treatment of short bowel syndrome (SBS). This designation is granted to therapies intended to treat serious rare conditions affecting no more than five in 10,000 persons in the European Union and for which either no satisfactory treatment currently exists or the proposed therapy would provide a significant benefit to those affected compared with existing therapies.November 21, 2018 — Nestlé Health Sciences has partnered with Entrinsic Health Solutions on enterade, an electrolyte beverage designed to help address hydration issues in individuals with gastrointestinal (GI) issues related to cancer or chronic GI illness.
November 19, 2018 — The US Food and Drug Administration (FDA) has accepted the filing of a new drug application (NDA) for extended use of teduglutide injection in children aged 1 to 17 years with short bowel syndrome (SBS). Teduglutide is currently approved for adults with SBS who are dependent on parenteral nutrition.
November 19, 2018 — The US Food and Drug Administration (FDA) approves antibiotic rifamycin (Aemcolo) for the treatment of adults with traveler’s diarrhea caused by non-invasive strains of Escherichia coli (E. coli).
Treatment News Presented at ACG 2018
In October 2018, IFFGD gathered with clinicians, researchers, drug developers and manufacturers, and others at the American College of Gastroenterology (ACG) annual meeting in Philadelphia, PA to get the latest research updates in the field of digestive health. Major medical meetings, like ACG, present companies with an opportunity to share news on developments in drug treatments. Here are a selection of drug developments announced at ACG this year:
Long-term safety data was presented for the drug tenapanor for irritable bowel syndrome with constipation (IBS-C). In several previous Phase III trials, tenapanor was found to effectively reduce constipation and abdomial pain in patients with IBS-C. The most common side effect of the drug is diarrhea (9.2%).
Clinical data showing improvement in health-related quality of life and the effects on esophageal erosions were presented for IW-3718 for the treatment of persistent gastroesophageal reflux disease (GERD). Persistent GERD is defined as the persistent occurrence of heartburn and regurgitation despite standard treatment of proton pump inhibitors (PPIs). Phase III clinical trials are currently undergoing to assess the safety and effectiveness of IW-3718.
Safety and efficacy data were presented for plecanatide for the treatment of IBS-C and chronic idiopathic constipation (CIC) in patients 65 years and older compared with patients younger than 65 years. Safety (adverse event and discontinuation rates) and efficacy were consistently demonstrated between the two populations.
Results of a two year follow-up study confirm safety and tolerability of a novel delivery of peppermint oil for the dietary management of IBS. The most common self-reported side effects were abdominal pain/discomfort/distension, diarrhea, and dyspepsia.
Safety and effeicacy data were presented for eluxadoline in patients with IBS with diarrhea (IBS-D) who reported inadequate symptom control with over-the-counter (OTC) loperamide. Eluxadoline is not indicated for patients without a gallbladder.
Overall safety and tolerability data were presented for the drug relamorelin for the treatment of adults with diabetic gastroparesis.
The availability of a new blood test for the diagnosis of IBS-D (detects elevated levels of Cyolethal distending toxin B (CdtB) and anti-vinculin in blood) was announced.
A two-week course of rifaximin was found to improve abdominal pain and bloating symptoms in adults with IBS-D.
Improved bowel regularity, symptom improvement, and patient satisfaction were reported for a new prebiotic fiber supplement for generalized constipation.
September 18, 2018 — Teduglutide has been approved in South Korea by the Ministry of Food and Drug Safety for the treatment of short bowel syndrome (SBS).
September 18, 2018 — Linaclotide (Linzess) has been approved in Japan for the treatment of adult patients with chronic constipation.
September 18, 2018 — The US Food and Drug Administration (FDA) has accepted a new drug application (NDA) for an investigational nasal spray formulation of metoclopramide (Gimoti) for the treatment of adult women with acute or recurrent diabetic gastroparesis.
December 16, 2015 — The new FDA approved drug, eluxadoline (Viberzi), is available for the treatment of irritable bowel syndrome with diarrhea (IBS-D) in men and women.
